
Waiting for approval or even requesting for Medicaid to cover weight loss surgery can be nerve wracking, even more so for those who are eager to have the surgery done and become a healthier version of themselves.1
The timeline of approval, which could take up to 3 months, will depend on a number factors which will ultimately be influenced by the requirements set by the Medicaid such as passing a psychological exam, having a high enough BMI or whether a candidate for surgery has documentation stating surgery is a medical necessity—the prerequisites for Medicaid will typically vary from other insurance companies.
While Medicaid can take up to 90 days to approve the application, the information below goes over the necessary screenings and requirements set by Medicaid, common delays, the types of weight loss surgeries that Medicaid covers and what can be done if Medicaid denies the surgery.
Medicaid Coverage for Weight Loss Surgery (Bariatric Surgery)
Medicaid may cover weight loss surgery (bariatric surgery) for individuals diagnosed with severe obesity (morbid obesity), provided they have a qualifying health condition such as diabetes, are medically cleared for surgery, and have made attempts with prior weight loss methods and treatments. Eligible procedures under consideration include gastric bypass, sleeve, and band surgeries, once all necessary criteria are fulfilled.2
- Gastric Sleeve Surgery—This surgery entails the removal of some parts of the stomach to prevent someone from eating at the same levels they would be before, and as a result end up feeling full sooner.
- Gastric Bypass—In addition, Medicaid pays for gastric bypass surgery which involves the top part of the stomach being joined to the small intestine which makes an individual feel satiated sooner while preventing the absorption of calories.
- Lap Gastric Band Surgery—In this type of surgery, a band is placed around the stomach which allows someone to not eat as much as food to feel satiated.
Although various weight loss surgeries are available for individuals who have exhausted all options before quitting weight loss programs, Medicaid only covers the following common procedures.
If a different type of surgery is being sought, then different insurance coverage such as Anthem bcbs health insurance should be obtained or paying out of pocket for the procedure.
Medicaid typically has two types of coverage:
- Mandatory Medicaid Benefits—This includes obesity screening for beneficiaries below the age 21.
- Optional Medicaid Benefits—These include weight loss interventions, weight loss drugs, education and counseling.
The requirements for Medicaid to bear the costs of surgery include being of a minimum age and documentation proving someone has participated in a weight loss program that is medically supervised.
What Are the Medicaid Requirements for Bariatric Surgery?
Individuals interested in weight loss surgery under Medicaid must meet specific criteria, including demonstrating a medical necessity for the surgery and meeting certain BMI thresholds.
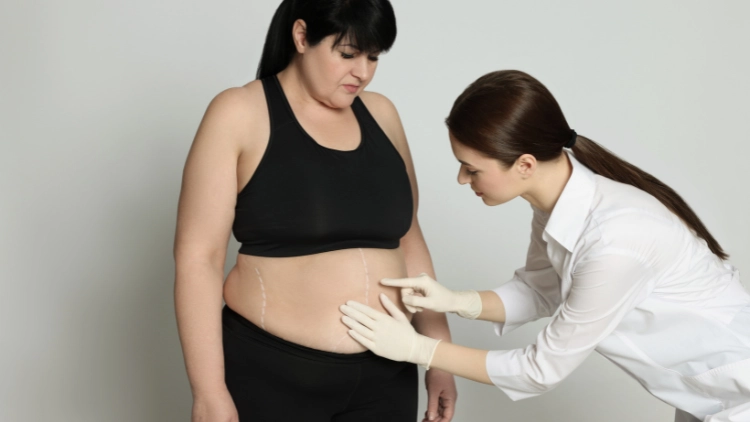
Source: Africa images via Canva.com3
- Having a body mass index (BMI) equal to or exceeding 35 and having another health related condition (comorbidity) such as high blood pressure, sleep apnea, diabetes and high cholesterol. BMI is an indicator of body fatness in individuals.4
Individuals who are under 21 should have a BMI of 40 coupled with a comorbidity. - Male and female who are over the age of 15 or 13 respectively.
- Passing a psychological exam.
- Letter from a doctor stating that the candidate medically requires surgery to maintain healthy weight levels.
- Documentation showing that the candidate is unsuccessful in treating their conditions with standard treatment.
- Ensures that the candidate understands that the surgery is life changing and that they will have to permanently alter their diet and lifestyle post-surgery.
- Proof of participation (documented) in a weight loss program or one of the trending diets that is medically supervised with a duration of 6 months. This program needs to take place within 12 months of the surgery.
- There are services that will be available to the candidate—these include nutritional and psychological services both pre and post-surgery.
Medical History & Physicals Before Approval Is Considered
There are several physicals that will need to be performed on candidates as well as establishing what their medical history is including blood tests and pulmonary function tests.
Beneficiaries should expect to have the following tests to get a detailed picture of their health:
- Chest x-rays
- Blood tests
- Liver function tests
- Obtaining a cardiac clearance
- Electrocardiogram (EKG)
- Echocardiogram (ECG)
- Sleep pattern studies
- Pulmonary function tests
- Upper gastrointestinal evaluation and tests
In addition to these tests, these medical histories as well as psychological evaluations are performed due to the impact the surgery will have on the relationship with food on the beneficiary:
- Determining the previous attempts to lose weight and what the results were after 2 years; bariatric surgery is the therapy of choice and generally last resort for individuals with severe obesity.5
- Current dieting behaviors
- Physical activity levels
- Dieting and weight history
- Status of current psychological function
- Mental health history, current treatment, diagnoses and determining current status
- Substance (drugs) evaluation
- Tobacco use should cease at least 6 weeks before surgery and it is strongly recommended to quit smoking after the procedure
- Cognitive status and abilities
- Establishing and determining their social support system
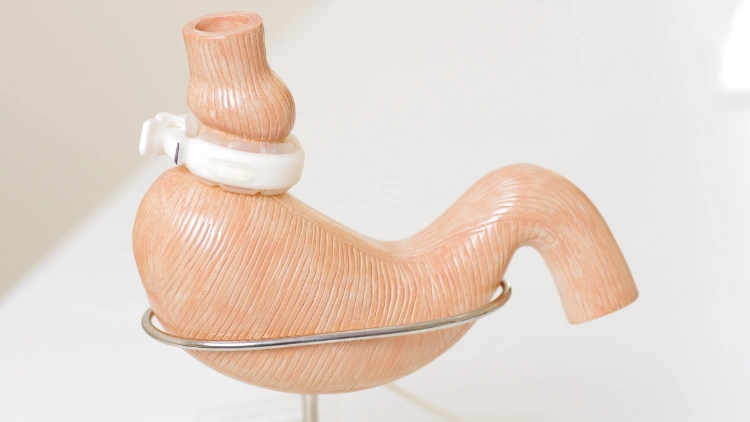
Source: Capifrutta via Canva.com6
Oftentimes, candidates who have had challenges following weight loss rules and are now in need of weight loss surgery will also meet with surgeons to discuss the best surgery option for them offering the best benefits.
They will also be made to understand and sign a form informing them of the potential, but rare risks associated with bariatric surgery.7 Risks include, but are limited to:
- Dilation of the esophagus
- Infections
- Gallstones
- Blocked opening of the stomach pouch
- Leakage of food in the case of the gastric band slipping out of place
- Acid reflux
- Obstruction of the stomach
- Inability to eat some types of foods etc.
Is It Hard To Get Medicaid Approval for Weight Loss Surgery?
Getting approval for Medicaid to approve weight loss surgery is not necessarily hard, as long as all requirements are met.
BMI needs to be at the aforementioned levels and the beneficiary must have an accompanying condition such as high blood pressure in addition to the requirements set forth above.
Most people get their applications denied because they fail to meet one or several of the criteria specified by Medicaid. They may also omit some information required when submitting their applications, resulting in a denial.
Approval Timeline for Medicaid Weight Loss Surgery
After all requirements and conditions are met, applicants have to play the waiting game. Once the application, evaluations and tests are complete, beneficiaries can expect to have their applications approved or denied after 90 days of submitting all the necessary documentation.
Common Reasons Why Medicaid’s Approval or Denial Is Taking So Long
There are a number of reasons why Medicaid may deny an application including not meeting the requirements such as having a chronic disease like cancer or being pregnant.
Even minor omissions of information required could mean that it can take additional weeks for the application to be re-determined and/ or any denial decision overturned.
This will undoubtedly add to the typical timeline of approval.
With that said, in addition to a failure to meet the requirements required set by Medicaid, some of the common reasons for denial include:
- Having a current pregnancy
- Bowel disease (inflammatory)
- Steroid use that is long term
- Malignant cancer
- Psychological treatment which will have an impact on post-surgery lifestyle changes
- Pancreatitis (chronic)
Tests & Screenings Necessary Once Medicaid Approves Candidates for Weight Loss Surgery
Once Medicaid surgery is approved, beneficiaries will have to undergo some tests and screenings that need to be carried out which include pulmonary (lungs) and thyroid function tests. Candidates should expect the tests below:
- Medication list (medicines being taken by the beneficiary)
- Having a negative pregnancy test before the surgery
- Blood pressure
- Establishment of previous noncompliance with medical treatment
- Thyroid function tests
- Cardiology tests
- Chest radiographs
- If candidates are on estrogen therapy, this is discontinued
- Evaluation of the lungs (pulmonary)
- Deep venous thrombosis diagnostic evaluation
- Viral hepatitis screen
- Abdominal ultrasonography
- Glycemic control optimization
- Establishment from the medical records that any morbidity is not an indication for the surgery
How Do I Find Doctors & Locations That Accept Medicaid for Weight Loss Surgery?
Medicaid beneficiaries who have approval for weight loss surgery must have their surgeries done at a Bariatric Center for Excellence—these are facilities with high levels of excellence in bariatric surgery.
This accreditation ensures that beneficiaries have a guarantee of the best possible treatment.
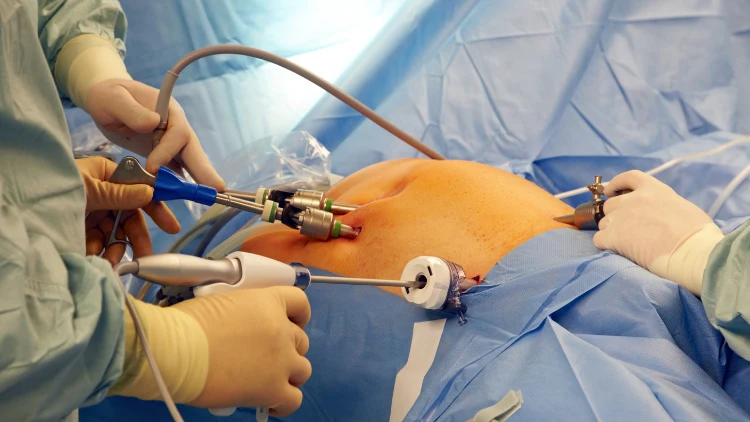
Source: thelinke via Canva.com8
To find these facilities by state and doctors that accept Medicaid for weight loss surgery, obtain contact information from Medicaid directly via the Medicaid program contact page and/ or their contact us page to query locations and doctors who perform bariatric surgery.9, 10
The Bariatric Surgery Process: Preparation, Day of Surgery & Recovery
Once gastric bypass surgery with Medicaid or any other of the two surgeries is approved, there are some final steps that will be taken in preparation of surgery. These include:
Scheduling Surgery—The coordinator from the health institution will work with the beneficiary to set a date and time for surgery and prepare for the final steps.
Review of Expectations—Beneficiaries will be given a review of the type of diet they will expect to have after the surgery. Following the recommended diet is critical for a successful outcome of the surgery and is a lifelong change.
Day of Surgery—On the day of surgery, candidates should expect to have general anesthesia administered which means they will be asleep for the entire procedure. Beneficiaries should expect to spend 1-3 nights at the hospital after surgery is completed.
The surgeries completed are state of the art and apply the latest advanced minimally invasive techniques. Surgeries are either done robotically or through laparoscopy—surgical procedure that gives access to the inside of the abdomen with a small incision.11
These types of surgeries are beneficial as they allow smaller scars and make recovery a faster and easier process. In some cases, patients are able to walk and sip on fluids on the same day as the surgery.
After Surgery & Recovery—Candidates should assist the healing process by avoiding lifting anything more than 10 lbs. 4-6 weeks post-surgery. Abdominal exercises such as push-ups and sit ups should also be avoided in the 6-8 weeks after surgery.
Follow up visits after the surgery to monitor patient wellness and keep track of recovery and progress happens at a number of time intervals including:
- 10-14 days
- 6 weeks
- 90 days
- 120 days
One year after surgery, check-ins are typically lowered to annual visits which last a lifetime. These visits are generally attended by a surgeon and/or nurse and a dietician.

Source: SHOTPRIME via Canva.com12
These measures are crucial to help the beneficiary maintain weight loss progress, prevent future weight gain, address surgery-related complications, and assess for any nutritional deficiencies.
What Should I Do if Medicaid Denies My Request for Weight Loss Surgery?
Pre-approvals for weight loss surgery with Medicaid doesn’t guarantee coverage, but in some situations, candidates may receive outright denials for weight loss surgery—in cases like this, the best course of action would be to contact Medicaid to determine the reason for denial by making a request to have the denial in writing with reasons clearly stated.
Candidates can then contact their health provider who will analyze the reasons and either submit an appeal or a response to the same.
Weight loss surgery is often a last resort and life-changing procedure for many. For individuals on Medicaid, the approval process typically takes approximately 3 months. This timeline, however, depends on meeting and submitting the requirements set forth by the insurance agency in an organized and appropriate manner.
Frequently Asked Questions
Is Weight Loss Treatment Included in Medicaid Coverage?
Yes, Medicaid does cover a number of weight loss programs. Some are mandatory benefits such as obesity screenings and weight loss surgery after requirements are met. There are other benefits that are optional and vary from state to state such as weight loss pills, weight loss counseling and education. Gym membership and wellness programs may also be covered by some state programs.
Is Weight Loss Surgery Easier To Get Approved Through Medicaid or Regular Insurance?
Recent trends show that it is easier to get approved through regular insurance than Medicaid for weight loss surgery. In addition, uses of this public insurance are paying more out of pocket in comparison to their counterparts who use regular insurance.
What Is the Approval Time for Medicaid Coverage of Sleeve Gastrectomy Surgeries?
The approval time for weight loss surgeries, including procedures like sleeve gastrectomy, is usually around 90 days after submitting all necessary documents and test results.
What Are the Weight or BMI Requirements for Weight Loss Surgery?
Candidates who are over the age of 21 years should have a BMI that is over 35 and 40 for those that are under 21 years of age.
What Is the Cost of Weight Loss Surgery With & Without Insurance?
The average cost of weight loss surgery (bariatric surgery) varies between $8000 and $35000 before insurance coverage. Many insurance coverages will cover the cost for the surgery meaning there is little to no cost to the beneficiary. Bariatric surgery inside the U.S and Canada is costly compared to foreign countries such as Mexico.
How Do I Speed Up or Expedite the Medicaid Approval Process for Weight Loss Surgery?
Candidates frequently inquire about the timeline for bariatric surgery approval and whether it can be expedited. Unfortunately, there is no method to accelerate the Medicaid approval process for weight loss surgery. However, staying organized and ensuring all necessary documentation is submitted can help avoid delays in the approval process.
They should contact Medicaid and establish what exactly the requirements are, liaison with their bariatric coordinator to perform any preliminary verifications and compile the documents quickly and thoroughly leaving no omissions out.
References
1Kameleon007. “medicaid.” Canva. Accessed 27 April 2023. <https://www.canva.com/photos/MAEENCYPBiw-medicaid/>
2Medicaid, N. (2023). Medicaid and Health Choice. Retrieved from <https://files.nc.gov/ncdma/Public-Comment---1A-15-CT-Surgery-for-Clinically-Severe-or-Morbid-Obesity.pdf>
3Africa images. “Doctor Consulting Obese Woman on Light Background. Weight Loss Surgery.” Canva. Accessed 27 April 2023. <https://www.canva.com/photos/MAFKSbd5p3E-doctor-consulting-obese-woman-on-light-background-weight-loss-surgery/>
4Prevention, C. f. (2022, June 3). Body Mass Index (BMI). Retrieved 2023, from <https://www.cdc.gov/healthyweight/assessing/bmi/index.html>
5Pories, W. J. (2008, November). Bariatric Surgery: Risks and Rewards. Retrieved 2023, from <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2729256/>
6Capifrutta. “Lap-Band placed on a replica stomach.” Canva. Accessed 27 April 2023. <https://www.canva.com/photos/MAEEYehJhNA-lap-band-placed-on-a-replica-stomach/>
7Irene T. Ma, J. A. (2015, August). Gastrointestinal Complications After Bariatric Surgery. Retrieved 2023, from <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4843041/>
8thelinke. “Laparoscopic surgery.” Canva. Accessed 27 April 2023. <https://www.canva.com/photos/MAEJGUUBzsY-laparoscopic-surgery/>
9Medicaid. (2023). Beneficiary Resources. Retrieved 2023, from <https://www.medicaid.gov/about-us/beneficiary-resources/index.html>
10Medicaid. (2023). Contact Us. Retrieved 2023, from <https://www.medicaid.gov/about-us/contact-us/index.html>
11Medicine, N. L. (2023, March 6). What is a laparoscopy? Retrieved 2023, from <https://medlineplus.gov/lab-tests/laparoscopy/>
12SHOTPRIME. “Woman on a Weight Loss Diet Large Pants Measuring a Slim Figure.” Canva. Accessed 27 April 2023. <https://www.canva.com/photos/MAEJGiiFF5I-woman-on-a-weight-loss-diet-large-pants-measuring-a-slim-figure/>